Low back pain (LBP) is a condition that affects millions of people each year. It is the leading cause of disability worldwide and the condition for which the greatest number of people may benefit from rehabilitation.
Al Kozar, DO, knows a little something about LBP.
Dr. Kozar is a professor of Osteopathic Manipulative Medicine and sports medicine at VCOM-Virginia. He is also a practicing physician at the VCOM Sports & Osteopathic Medicine practice in Blacksburg where he regularly treats patients suffering from LBP. He points out that chronic back pain can have a major impact on the quality of life because in addition to biological and mechanical challenges, it also has psychosocial implications. “Everybody responds differently, based on their upbringing and how their family addressed pain and how much the pain affects their ability to do their work or their daily activities,” he says. “We often put up with back pain until it prevents us from doing those things. But pain tells us there is dysfunction somewhere in the musculoskeletal system.”
Dr. Kozar is collaborating with Vincent Wang, Ph.D., director of Virginia Tech’s Orthopedic Mechanobiology Laboratory, on two research projects to better understand the causes of back pain and how to treat it more effectively.
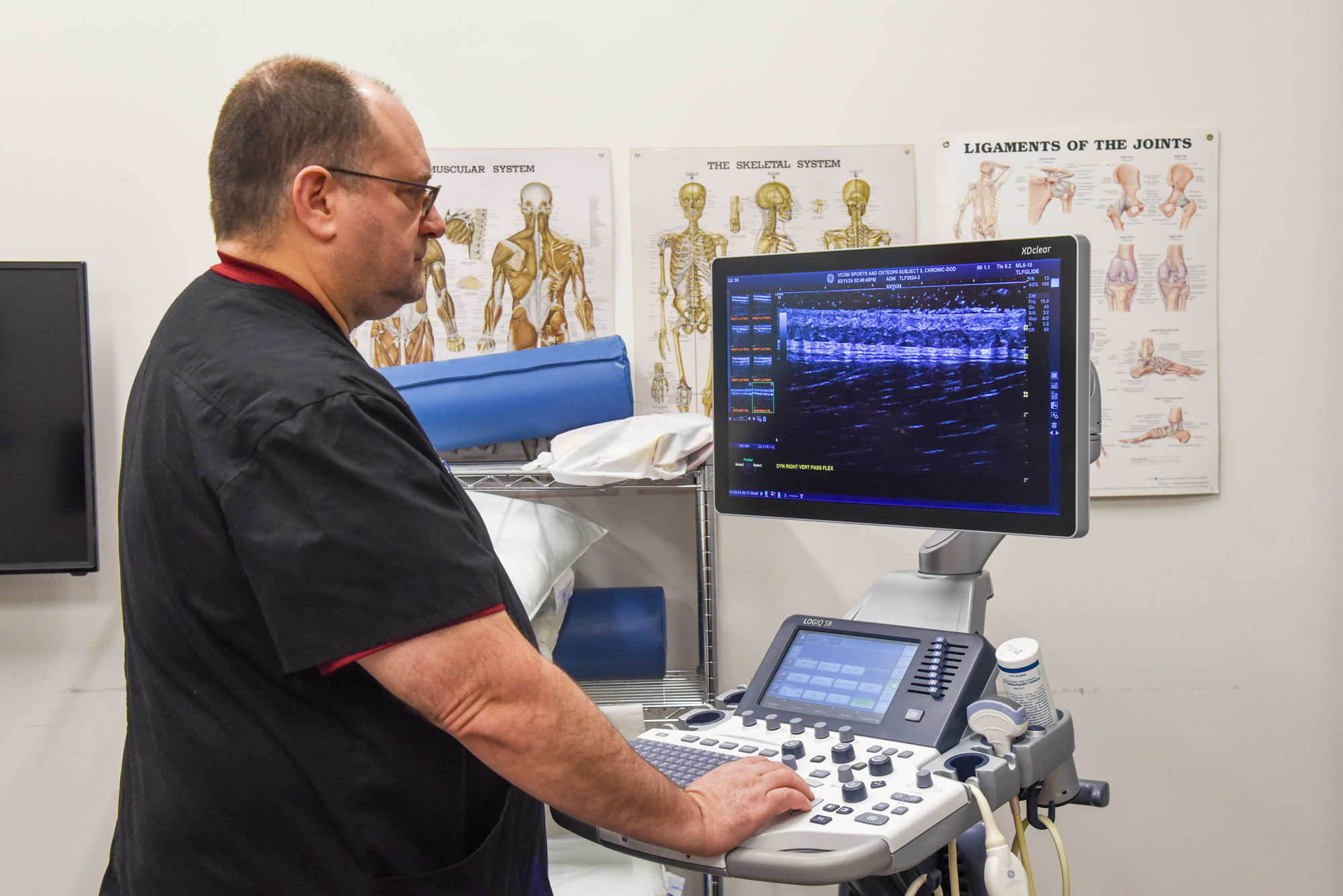
Like Dr. Kozar, Wang is an expert in the musculoskeletal system. His laboratory in Virginia Tech’s Department of Biomedical Engineering and Mechanics has received millions of dollars in funding to “support a variety of projects related to skeletal soft tissue biomechanics, repair, and healing.” The new research will build on recent advances in Wang’s lab and will include faculty and students at both VCOM and Virginia Tech. The researchers will recruit people who have LBP, as well as people who don’t, to perform ultrasound imaging on their thoracolumbar fascia (TLF). Ultrasound is a useful diagnostic tool, in part because it does not use ionizing radiation, is inexpensive and is effective in detecting soft tissue changes.
The TLF is integral to body movement. It has an important mechanical function in enabling us to bend over and pick things up, and it is a proprioceptive structure, meaning that it helps our bodies sense movement, action and our location in space. Dysfunction in this large soft tissue complex may be a frequent cause of LBP. However, TLF is also incredibly thin—only about 5 mm thick—so its injury is difficult to diagnose clinically. Medical imaging techniques such as ultrasound allow physicians and researchers to more effectively investigate changes not only to a patient’s TLF structure but also the glide motion within the layers of the TLF.
The teams are partnering on two funded projects related to diagnosing and treating LBP. The first project will take 24 months and is being funded by the United States Department of Defense (DoD) because service members and veterans often suffer from LBP due to the nature of their work. The DoD funding will enable the teams to study the effectiveness of a novel treatment called hydrodissection, which involves using ultrasound guidance to apply a dextrose solution to the TLF to separate its tissue layers and restore any glide restriction that might be contributing to causing a patient’s pain.
Additional funding from the American Osteopathic Association will enable an 18-month study on how osteopathic manipulative treatments can do essentially the same thing—relieve the restriction in the TLF.
Dr. Kozar anticipates that he will spend more than 1,500 hours over the next two years using ultrasound to acquire images of patients’ TLF. Wang’s research team will then perform detailed computer-based image analyses to help them quantify lower back flexibility and examine potential relationships between pain, function and imaging metrics. In addition to using conventional image analyses, the researchers will develop artificial intelligence approaches to objectively determine whether an image is from an individual with LBP.
“We hope these tools will further facilitate and improve clinical diagnosis, treatment and care of patients—not just within our group, but more broadly among clinicians and researchers in the field,” Wang says. Their research is particularly important because, he observes, “LBP can be experienced at any age, and we see these projects as valuable opportunities to extract valuable information from TLF ultrasound images in a manner that hasn’t been done before.”
Dr. Kozar’s team will study the clinical efficacy of osteopathic manipulative treatments and track patients over time. “We will be testing some physical exam maneuvers to see if they will be able to predict that a patient’s pain is being caused by TLF as opposed to something else,” he says. Dr. Kozar has been using these maneuvers for several years and the research will help him understand their effectiveness at predicting an issue with a patient’s TLF.

For years, we taught that an acute episode of back pain would go away in a couple of days, and it was nothing to worry about, but that’s not true at all. For 65-85% of people, those episodes get closer together, and they eventually end up with daily chronic pain that can be debilitating. I think it is important to view back pain as a progressive disease that can be altered and stopped.
In addition to developing effective treatments for LBP, the research may be able to prove to entities like insurance companies that there are evolving technologies that are useful for patients and that physicians should be able to use them. The more treatments that are covered, the more patients who can be treated.
Although VCOM is an independent medical school, the faculty and researchers at the College’s four campuses—in Blacksburg, Virginia; Spartanburg, South Carolina; Auburn, Alabama; and Monroe, Louisiana—have productive and meaningful research partnerships with colleagues at other institutions like Virginia Tech and Auburn University.
Dr. Kozar and Wang, who have already worked together for several years on tendon studies, are eager to expand their collaboration to similar tissues like the TLF. “[Physicians] do a lot of things clinically, but we don’t always know how they work,” Dr. Kozar notes. “I don’t have the capacity to conduct mechanistic studies, so we need somebody to partner with us to look at those things.”
“Collaborations are vital,” Wang said in 2022. “I pursue what I regard to be highly important and timely clinical topics, but I’m not a physician. Combining expertise is how we address these challenges and hopefully improve others’ lives.”
Study Participants Needed
Study participants are needed for this research. If you are between the ages of 18 and 50—whether you have LBP or not—you might qualify to particpate. Read full details and find out how to participate.